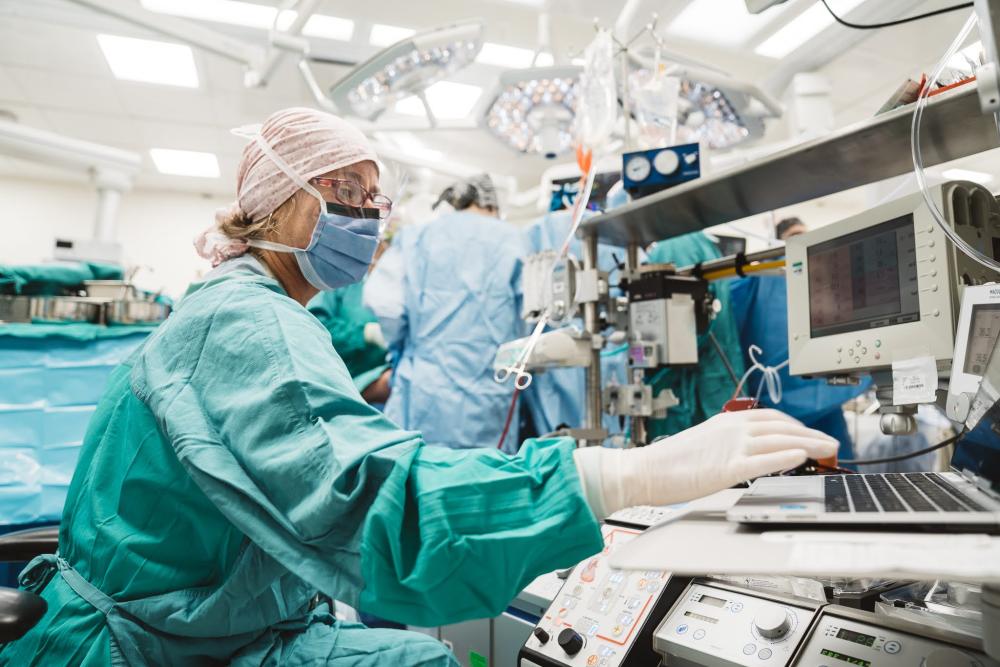
Unless you’ve experienced it first-hand, it’s likely many of us take heart surgery for granted. But consider for a moment, the role of our heart, continuously pumping blood through our bodies to provide our brain and organs the necessary oxygen and nutrients. Now, imagine stopping it long enough to be operated on or replaced altogether, and somehow still being kept alive. This is where perfusionists come in.
With an array of screens, pumps and tubes to monitor, perfusionists manage the device which essentially steps in as a person’s heart and lungs during cardiac surgery. However, Canada finds itself facing a drought of perfusionists.
“There’s always been a limited number of perfusionists across the country,” says Chris McKay, clinical perfusionist at London Health Sciences Centre (LHSC). “But as people retire, or find positions closer to their hometowns, LHSC has seen an exodus of these specialists over the last five years.”
Anticipating what lay over the horizon, LHSC’s interim director of cardiac care, Rachel Rushton, along with Chris, sat down with their team to discuss strategies for combatting the shortage. Together, they chose to create an initiative to sponsor individuals who enrol in the cardiovascular perfusion program at the Michener Institute of Education.
“Michener only has about 15 seats with hundreds of applicants every year,” Rachel says. “It’s incredibly competitive.”
After receiving financial support toward tuition and auxiliary fees, graduates of the program commit to four years at LHSC. Funded entirely by donors of London Health Sciences Foundation (LHSF), the first intern is set to graduate in spring 2023. And recognition of this need is growing, as more donors have shown interest refilling the pool of perfusionists at LHSC.
“There’s always a perfusionist and a backup perfusionist for every case involving heart surgery,” Rachel explains. “We really need to build a robust, local workforce to help improve the work/life balance.”
Apart from the heart-lung machine, perfusionists are responsible for initiating and maintaining any ventricular assist device (VAD): heart pumps implanted into a patient temporarily while they await surgery or therapy. And should someone experience excessive blood loss during surgery, a perfusionist is brought in to help salvage, wash and return it to the patient. In short, without them, the cardiac surgery program simply couldn’t function.
Chris says, after 21 years, she still feels the rush of adrenaline when she’s assisting with surgery. It’s about keeping patients alive while at the same time providing surgeons with an environment conducive to a successful procedure.
“There’s no other feeling like saving another person’s life,” she says, her voice infused with the passion of someone who loves their job.
The unsung heroes of cardiac surgery, perfusionists are masters of manipulating blood flow. And as demand outpaces the number of individuals qualified to provide service, wait times will lengthen and the standard of care will suffer. What’s needed now is to increase the flow of personnel coming into the department because when it comes to the art of life support, balance is everything.
